For years I thought that line was a joke. I’ve heard it in Sir Henry at Rawlinson End in all its incarnations — record, film and book. Drunk, mad old Sir Henry is the führer of Rawlinson End and is daily assisted to intoxication by Old Scrotum (the wrinkled retainer) and the unhygienic housekeeper Mrs. E. Mrs. E. chatters endlessly to herself about disgusting diseases from tapeworm to lice and in a random aside she ejaculates, “‘E got anthrax orf ‘is shaving brush, dear. The bristles were made of horse-hair.” An understandable mistake. When I Googled it for context I was flabbergasted to discover articles from the Journal of the American Medical Association describing this exact malady. It was real. It happened. People got anthrax from shaving.

The whole health scare over anthrax started in World War I. People at the time shaved with a shaving brush, which they used to lather the soap and apply it to their face. These brushes were supposed to be made out of badger hair, but there were a lot of cheap knock-offs made out of horsehair or pig bristles instead: “The large majority of the so-called badger-hair brushes now on the market are really clever imitations made by treating white hair or bristles by secret processes.”1 The United States got its supply of horsehair from Russia, China and Japan by way of Europe where the horsehair was treated and disinfected. That was until the war disrupted supply lines and the horsehair had to come via the Pacific Ocean, where the cleaning procedures weren’t so well established. Little did innocent barbers know the terrors that lurked in their shaving brushes.
Anthrax is a telluric bacterium, which means it naturally occurs in the ground. It gets picked up by farmyard animals and spread to humans via the animals’ hair and hides. Astute readers will see where this is going. The naturally-occurring anthrax in horses combined with poor disinfection meant boatloads of anthrax-ridden shaving brushes were being shipped around the world.
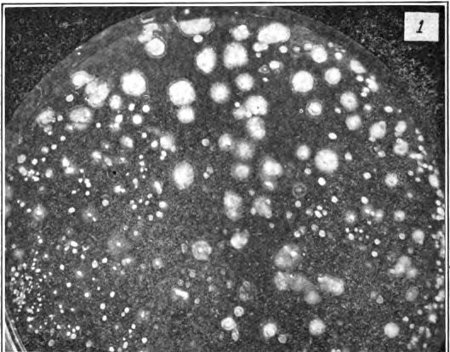
Cases of anthrax infection started to break out in 1915. Cases sprung up in England and Ireland, closely followed by New York later that year. New York appears to have been the center of the American anthrax outbreaks. Dr. Symmers of Bellevue Hospital described the progress of the disease using the case of Frederick Post, a prominent polo player:
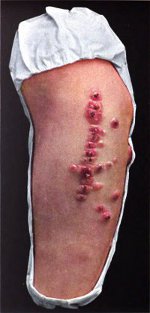
Anthrax, at the outset, is manifested by a characteristic lesion at the point of inoculation. This usually is on the face, as in Mr. Post’s case. It looks like an ordinary pimple, red and itching. Within a day or so the pimple breaks down into a large, blackish ulcer, surrounded by an enormous but painless swelling. That one pimple and swelling is all the visible sign there may be of the disease. But, if the swelling is on the cheek, as in Mr. Post’s case, it may be enormous, closing the eye.4
The entire disease could take its course in a matter of days. Professor Ellermann of the University of Copenhagen went from pimple to grave between December 17 and December 24 1924. The man died on Christmas Eve from anthrax on his shaving brush. In no way does that sentence deserve to make sense. And yet from 1915 to 1921, 50 cases of shaving-brush anthrax occurred in England, resulting in 18 deaths. New York alone produced 18 cases of shaving-brush anthrax between 1919 and 1920. Nine of those patients died, and all because they wanted to trim their whiskers. The New York City Department of Health conducted research on horsehair brushes and discovered a staggering 80% of them to be contaminated with anthrax spores. A similar study, however, by Bellevue Hospital tested 41 brushes and only discovered virulent anthrax in only 7.3% of them. The former study does not mention their sample space, so it’s hard to compare the results, but “sunny with a 7.3% chance of anthrax” is a poor forecast any day.
By 1920 the New York Department of Health had jumped on the problem and issued strict regulations for sterilization and sales. Hair products had to be sterilized by boiling or autoclave, and could only be sold if it had the word “sterilized” printed on the packaging. The shock public awareness and government regulations strangled the anthrax problem quite effectively, although isolated outbreaks would continue for the next few decades wherever a dodgy shipment of shaving brushes could be found. The decline of shaving brushes means you’re unlikely to get anthrax now, and improvements in antiobiotics means you’re even less likely to die from it. Doctors and government regulators, big-wigs with fancy degrees, like to claim the credit for banishing anthrax from the modern world. However I would ask you to take a moment and spare a thought for Mrs. E., the unhygienic housekeeper of Rawlinson End, who was my very first champion of anthrax awareness.
Notes
Bibliography
-
“Anthrax from Shaving Brushes”. The American Journal of Public Health 15.5 (1925): 440. Print.
-
“Anthrax Not Fatal Says Dr. Symmers”. The New York Times 25 July 1920. Print.
-
Clendening, Logan. “Anthrax, Commonly Called ‘Wool Sorter’s Disease’“. The Windsor Daily Star 21 March 1939: 14. Print.
-
“An Investigation of the Shaving-Brush Industry, with Special Reference to Anthrax”. Public Health Reports 34.19 (1919): 994-995. Print.
-
Jacobi. Portfolio of Dermochromes. Trans. J. J. Pringle. New York: Rebman, 1903. Print.
-
Hubbard, S. Dana. “Anthrax in Animal (Horse) Hair”. The Journal of the American Medical Association 75.25 (1920): 1687-1690. Print.
-
Morris, Harry. “Carrion Feeders as Disseminators of Anthrax or Charbon”. Louisiana Bulletin 136 (1912): 4-16. Print.
-
Symmers, Douglas and Cady, D. W. “Occurrence of Virulent Anthrax Bacilli in Cheap Shaving Brushes”. The Journal of the American Medical Association 77.27 (1921): 2120-2121. Print.